Symptoms
Arthritis
Back Pain
Carpal Tunnel Syndrome
Headache
Knee Pain
Neck Pain
Pregnancy
Whiplash
Rotator Cuff Tendinitis
PainCare of San Diego
Office Hours
Monday 8:30 AM – 6:00 PM
Tuesday 8:30 AM – 6:00 PM
Wednesday 8:30 AM – 6:00 PM
Thursday 8:30 AM – 6:00 PM
Friday 8:30 AM – 6:00 PM
Saturday Closed
Sunday Closed
Book Your Appointment Today
(858) 202-1546
or
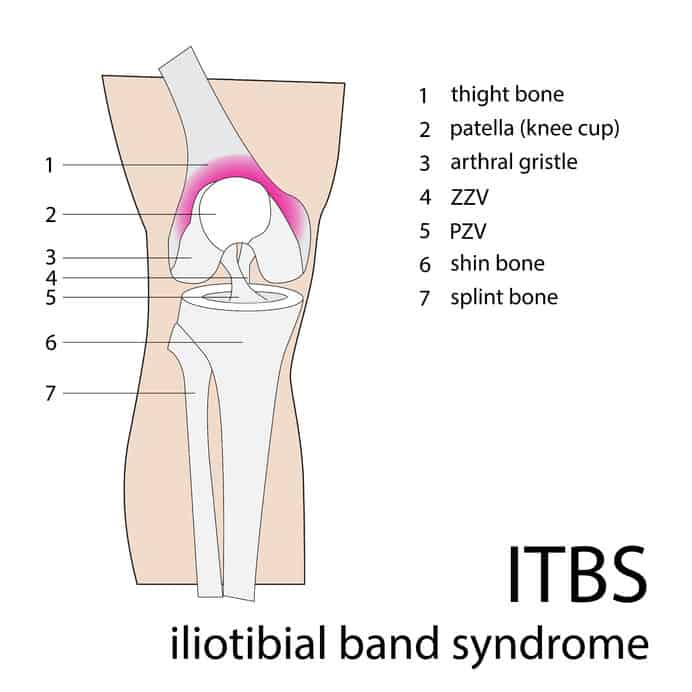
Iliotibial band friction syndrome
The iliotibial band is a thick band of tissue that extends from the thigh down over the knee and attaches to the tibia. When the knee bends (flexion) and straightens (extension), the iliotibial band slides over the bony parts of the outer knee (lateral femoral epicondyle). The term iliotibial band friction syndrome(ITBFS) refers specifically to a syndrome of lateral knee pain related to irritation and inflammation of the distal portion of the iliotibial band at, or just distal to, the point at which it crosses the lateral femoral epicondyle.
Iliotibial band friction syndrome is an overuse injury caused by repetitive friction of the iliotibial band across the lateral femoral epicondyle. It is a well recognized cause of knee pain in runners so it is commonly called “runner’s knee”, although the condition is not unique to runners, however, nor is lateral knee pain the only manifestation of iliotibial band injury. It is now frequently seen in cyclists, weight lifters, skiers and soccer players. It has also been found that injury to the iliotibial band and related structures may be noted as lateral “hip” or lateral thigh pain, as well as lateral knee pain.
Knee Tendonitis Symptoms
Our joints move by the power of your muscles. The muscles attach to your joints through tissues called tendons. The tendons transfer the force from your muscle across the joint and cause it to move. Sometimes this tendon becomes inflamed because it was injured (such as a direct blow to the thigh) or overused (such as biking up hills). When the tendon is inflamed, doctors add the ending “itis” and thus, we call this tendonitis.
Chronic cases are called tendonosis indicating chronic inflammation. In some cases, the tendon actually tears in half and this is called a tendon rupture. If you can not straighten your knee because of pain over your tendons, seek medical treatment immediately. Tendonitis pain is usually described as an ache that can be sharp with exiting from a chair or with squatting. The pain is usually improved with rest. Usually the patellar tendon in the front of your knee is most involved. This is called “patellar tendonitis” or “jumper’s knee”. Sometimes the pain can be so bad that even the weight of your bedsheets on your knee can irritate the pain.
Identifying the causes of the pain and inflammation and directing functional treatment have very good outcomes for this condition.
Patella-femoral Pain Syndrome
This disease is also known as softening of the cartilage of your knee cap or “anterior knee pain”. This is a big medical word for a condition where the shiny cartilage surface of your patella (knee cap) is softened due to many factors including abnormal pressure across the joint surface or hormonal changes in your body.
This pain is usually located over the front of your knee and is described as a deep aching pain. It is sometimes associated with swelling and is usually worse when your knee is bent for long periods of time such sitting in a car or bus. The pain is also worse with such activities as running, biking, squatting, kneeling or stair climbing (either up or down stairs).It is sometimes associated with mild or moderate swelling of the knee and some people report a grinding feeling in their kneecap. It is more common in younger females especially after a growth spurt where the knee must carry more weight.
Many times this problem can be due to muscular imbalance of the quadriceps muscle whereby the outer quadriceps is stronger than the inner quadriceps muscle and causes the knee cap to track up the thigh incorrectly. This cause irritation and inflammation on the undersurface of the knee cap and ultimately cartilage degeneration. It is usually pretty simple to diagnose the problem, but the key is to look at the feet first!
KNEE BURSITIS SYMPTOMS
Your body has sacks of fluid located in strategic places to allow your tendons to glide effortlessly over your bones. If you did not have a bursa, your joints would be painful with every movement. However, sometimes this sack of fluid becomes inflamed from either an injury (such as a direct blow to the knee), overuse (such as kneeling to scrub floors) or infection.
When the bursa becomes inflamed, doctors add the ending “itis” meaning inflammation. Thus, your bursa becomes bursitis. Usually bursitis produces a very specifically located swelling on your knee.
- Pes Anserine Bursitis is swelling located on the inside (medial) part of your knee along the upper part of your tibia. The pain of bursitis is usually sharp and worse with either touching the area or even when you sleep and the two knees touch each other. This typically happens in older patients.
- Patellar bursitis (or “pre-patellar bursitis”) is located over the front of the patellar ligament and kneecap (patella). The pain is located right in the front of your knee, and it can even be painful to have the bedsheets touch your skin in this area. This is the most common type of bursitis.
- An infection to the bursa usually has redness associated with this swelling and the pain is constant. If you think you may have an infection, please seek medical treatment immediately.
